Known as a tick-borne illness, Lyme disease affects 300,000 people in the United States with as many as 30,000 new cases reported annually. The debilitating symptoms of Lyme disease can significantly reduce a person’s capacity to work and care for themselves and loved ones. Lyme disease is considered one of the most complex bacterial infections leading to autoimmunity in which cells in the body attack healthy tissue. Let’s get a better understanding of how Lyme Disease is contracted, the difference between acute versus chronic symptoms, and how holistic approaches to treatment can facilitate recovery from Lyme disease.
Which Ticks Transmit Lyme Disease?
The disease is triggered by a bite from an infected black-legged tick (aka deer tick) which lives in wooded and grassy areas where it feeds on rodents and small animals that can carry Lyme. Even if you don’t spend time in the woods, a city can have a “tick hotspot” that can pop up in a park making it possible to pick up an infected tick.
The disease-carrying bite often comes from an “infant” tick (nymph) that’s about the size of a poppy seed. The nymph bite is not very painful. Most people won’t realize they’ve been bitten unless the sharper bite of the adult tick pierces their skin. The adult tick is also easier to see and remove before the disease is transmitted. Research shows that in most cases, a tick has to be attached to the skin for 24 hours or more for the bacterium that causes Lyme disease to be transmitted to human blood.
Symptoms of Lyme Disease
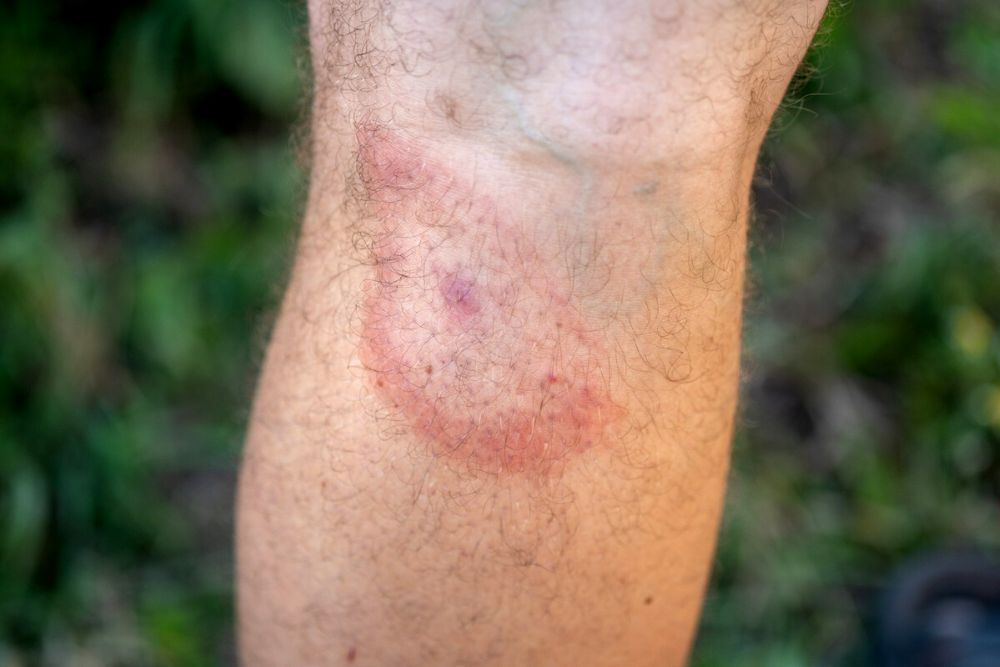
A person may have the tell-tale bullseye rash that appears on the skin after a tick bite, accompanied by flu-like symptoms. Research shows, however, that only about 30% of people with Lyme Disease had these “classic” symptoms–including the bullseye rash. Why might this be?
Bullseye rash (also called erythema migrans) can occur a week or longer after the bite. It is often characterized by a circular red center surrounded by a region of normal-looking skin and one or more outer red rings. Erythema migrans can also present as a solid, colored lesion without any rings.
One theory indicates that a strong immune system can keep Lyme disease in a dormant state in your body for months or years. Therefore, if you have symptoms, but not the classic bite mark, it’s best to request the diagnostic tests for Lyme Disease.
There is a difference between acute (or classic) symptoms and chronic symptoms of Lyme Disease. The acute symptoms a person may experience following a tick bite include:
- Bullseye rash
- Pain, sometimes heat at the bite area
- Headache
- Fever, chills
- Fatigue
- Dizziness
- Shortness of breath
- Neck stiffness
- Swelling
- Loss of muscle tone in the face (facial palsy)
- Muscle and/or joint pain
- Inflammation in the spinal cord and brain
If the disease has been dormant or was missed during the acute stage, a person can experience a great variability of chronic symptoms:
- Tingling, numbness, or burning sensations (nerve pain)
- Stiff or sore neck
- Sensitivity to light and sound
- Difficulty falling/staying asleep
- Problems with memory, concentration
- Depression/anxiety
- Chronic or intense flares of fatigue
- Debilitating pain that migrates around the body
- Variability in “good” & “bad” days, without changing self-care or medical regimen
Diagnosing Lyme Disease
If the bullseye rash is present, it is considered diagnostic for Lyme disease. If the bite is not present or questionable, a doctor will order specific tests including ELISA, Western Blot, Igenex, or others to test for the presence of the bacteria (B. burgdorferi) that causes Lyme disease. Antibodies can take weeks to develop so testing too soon can give a false-negative. If symptoms persist or change, the blood is re-tested.
Treating Lyme Disease
The standard mainstream treatment for acute Lyme disease is a course of antibiotics for 14 to 21 days. If the illness affects the central nervous system, intravenous antibiotics are typically given. Following antibiotic treatment, a person may have lingering health problems from the bacterial infection such as muscle/joint ache and fatigue or the development of an autoimmune condition. There may also be post-treatment complications from the antibiotic treatment such as fungal overgrowth and GI tract dysfunction.
Holistic treatment may include antibiotic treatment in addition to other therapeutics that help to support the body’s innate healing ability. In the case of Lyme, balancing the immune system response and supporting the detoxification process is also generally a focus. Depending on the patient’s individual needs, treatment plans may include medicine from a variety of therapeutics such as:
- Botanical (plant)
- Nutritional
- Homeopathic
- Chiropractic or other physical medicine
- Ayurvedic
- Supplements and IV
- Hydrotherapy
- Lifestyle: movement, stress management, sleep, and hydration
Regardless of the medicine used in the treatment plan, the holistic practitioner seeks to assist the body in its healing. The goals will be to provide what the body needs to thrive, strengthen the immune system, assist the body in detoxifying itself, and stimulate the innate healing ability.
People all over the world are successfully treated for Lyme using various approaches. If you suspect you have Lyme, check with your holistic health practitioner to arrange testing and to discuss treatment options.
Resources
LymeDisease.org. “About Ticks and Lyme Disease.” Accessed September 8, 2022. https://www.lymedisease.org/lyme-basics/ticks/about-ticks/
CDC. “How Many People Get Lyme Disease? | CDC.” Centers for Disease Control and Prevention, January 13, 2021. https://www.cdc.gov/lyme/stats/humancases.html
CDC. “Lyme Disease Data and Surveillance | CDC.” Centers for Disease Control and Prevention, August 29, 2022. https://www.cdc.gov/lyme/datasurveillance/index.html
Kugeler, K., et al. “Estimating the Frequency of Lyme Disease Diagnoses, United States, 2010–2018 – Volume 27, Number 2-February 2021 – Emerging Infectious Diseases Journal – CDC.” Accessed September 8, 2022. https://doi.org/10.3201/eid2702.202731
Singh, S. K., and H. J. Girschick. “Lyme Borreliosis: From Infection to Autoimmunity.” Clinical Microbiology and Infection: The Official Publication of the European Society of Clinical Microbiology and Infectious Diseases 10, no. 7 (July 2004): 598–614. https://doi.org/10.1111/j.1469-0691.2004.00895.x
CDC. “Diagnosis and Testing of Lyme Disease | CDC.” Centers for Disease Control and Prevention, May 21, 2021. https://www.cdc.gov/lyme/diagnosistesting/index.html
Wonk, Lyme Policy. “MyLymeData Viz – What Alternative Lyme Disease Treatments Work?” LymeDisease.Org (blog), January 7, 2019. https://www.lymedisease.org/mylymedata-alternative-lyme-disease-treatment/